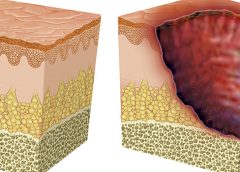
On April 13, 2016, the National Pressure Ulcer Advisory Panel (NPUAP) announced changes in pressure ulcer terminology and staging definitions. Providers can adapt NPUAP’s changes for their clinical practice and documentation, but it’s important to note that, as of press time, the Centers for Medicare & Medicaid Services (CMS) has not adopted the changes. This means that providers can’t use NPUAP’s updates when completing CMS assessment forms, such as the Minimum Data Set (MDS) or Outcome and Assessment Information Set (OASIS). Instead, they must code the CMS assessment forms according to current CMS instructions and definitions. In addition, there is no ICD-10 code for pressure injury. (more…)
Read MoreTag: definitions and terminology
A pressure ulcer by any other name
Just when we think we’ve figured out pressure ulcer staging, it changes again. In April 2016, the National Pressure Ulcer Advisory Panel (NPUAP) held a consensus conference on staging definitions and terminology. The purpose: to analyze and discuss the rationale for the panel’s changes. One of the key changes is replacing the term “pressure ulcer” with “pressure injury.” So instead of calling it a pressure ulcer staging system, NPUAP will refer to it as a pressure injury staging system. The panel explained that the new terminology “more accurately describes pressure injuries to both intact and ulcerated skin.” Other changes include: (more…)
Read More