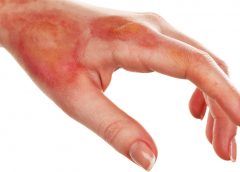
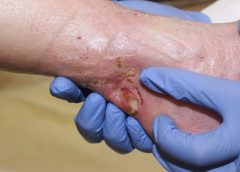
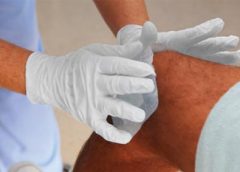
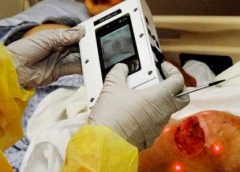
BioLab Sciences, an innovator in regenerative medicine technologies, has announced the patent of MyOwn SkinTM, a new, non-evasive, regenerative tissue therapy that uses a patient’s own skin to accelerate the healing of chronic wounds, burns, diabetic foot ulcers and other difficult-to-heal wounds.
Read MoreTag: chronic wounds
Topical gel containing blood pressure drugs shown effective in healing chronic wounds
An international research team led by Johns Hopkins University School of Medicine is seeking approval from the FDA for a topical gel they have created from oral blood pressure pills that has shown to be effective in the healing of chronic skin wounds in mice and pigs. A report of the team’s findings have been published in the Journal of Investigative Dermatology. Read more.
Read MoreBreaking silos: Effective wound healing means treatment across the continuum
Around 6.5 million patients in the U.S. suffer from chronic wounds, such as pressure injuries or ulcers. Treatment costs $25 billion each year, representing a sizable and growing problem. Despite the wide impact of chronic wounds, it’s rare to see specialized, effective wound care delivered across the care continuum.
A chronic non-healing wound is a surrogate marker for illness. These patients require holistic management of their co-morbidities and continuity across care settings.
Despite this, a great deal of emphasis has been placed on treating wounds as singular events, managed topically with expensive dressings and support surfaces. This is only a small part of wound healing.
As a physician focused solely on wound care, I have learned that we must shift the focus from simply treating the wound to treating the wounded patient. The impact in the post-acute care setting in particular is worthy of evaluation and discussion, as up to 29% of patients in long-term care facilities will experience a pressure ulcer, posing serious legal, financial, and staffing implications.
For those providers working outside long-term care, there is little understanding of challenges facing LTC providers. Acute providers do not often ask, for example, how are my LTC partners reimbursed? How are they staffed? What are the requirements and regulatory pressures they face? Asking these questions would facilitate a more productive dialogue with a focus on collaborative prevention, rather than waiting until a chronic wound occurs in the LTC setting.
Creating an integrated wound care community
To address the needs of the present and growing population of patients with chronic wounds, Healogics developed an integrated wound care community model, to coordinate the wound healing process across all care settings. The program utilizes Healogics Specialty Physicians, a subspecialty group of physicians and providers with extensive training solely focused on wound care.
HSPs provide expert inpatient consultation and ensure safe transition of patients out of the hospital into the appropriate care setting. Because HSPs see the patient regardless of post-discharge venue, patients receive the same quality of care whether they are going home, to a skilled-nursing, assisted living, or LTC setting. Because chronic wounds are surrogate markers for illness, we have realized it’s essential to have an integrated, multi-setting, and multi-disciplinary process to treat the patient and their co-morbidities.
Data collected at a pilot IWCC site in the Midwestern U.S. from 2014 to 2016 revealed very positive trends for chronic wound patients. In the acute care setting, the average length of stay decreased from 9.41 days to 5.64 days, and total cost of care per patient was reduced from $10,670 to $7,248.
We’re excited by these promising results, which were revealed at the American College of Wound Healing and Tissue Repair Conference last December. We look forward to refining and expanding the model by helping our partners in acute and LTC settings standardize their practices, use evidence-based clinical guidelines, mobilize technologies and processes, and pay critical attention to patient safety and value-based outcomes.
When it comes to wound healing, no venue of care should operate alone—an integrated solution that creates continuity for the patient is critical. There are four things LTC facilities can do to break down the silos:
Read more at McKnight’s
Read MoreWound Photography – How it Benefits Clinical Documentation
Accurate assessment and documentation of wounds is essential for developing a comprehensive plan of care. Photography now plays a key role in wound care. The use of digital photography has enhanced the reliability and accuracy of wound documentation. Though a wound assessment in patient files includes details such as location, depth, odor, condition of surrounding tissue and other details, a visual record can be worth even more.
Digital photography is becoming a more prevalent documentation tool. According to an article published in McKnight’s, forensic nursing experts recommend using photographs to document injury. The photos show both how an injury occurred and how it is healing.
The National Pressure Ulcer Advisory Panel (NPUAP) also supports photography as a more accurate means for assessment of wound dimensions and wound base over time.
A visual confirmation to the written record, these images:
- Facilitate better diagnosis
- Enhance clinical documentation
- Help to monitor the progress of wound healing
- Help prevent litigation in wound management
- Allow inter-disciplinary communication among the wound care team
Read more at Wound Wizard
Read MorePreparing the wound bed: Basic strategies, novel methods
The goal of wound-bed preparation is to create a stable, well-vascularized environment that aids healing of chronic wounds. Without proper preparation, even the most expensive wound-care products and devices are unlikely to produce positive outcomes.
To best prepare the wound bed, you need to understand wound healing physiology and wound care basics, as well as how to evaluate the patient’s overall health and manage wounds that don’t respond to treatment. (See Normal wound healing.) (more…)
Read More